There are lots of brain assessment tools commonly used for concussion, but they fail to consistently detect alterations in brain health.
The Brain Gauge system was designed to be used for a wide spectrum of neurological disorders and other situations that benefit from assessing brain health. From the beginning, we set out to design a system in which pre-injury “baseline” measures would not be necessary. After all, many clinicians see patients only after that patient has sustained a potentially concussive impact.
Similarly, it's difficult to approximate a patient’s brain health scores as they would have appeared before the onset of age-related dementia, or before the onset of a developmental disorder (which in theory, they are born with), or before the onset of chronic pain (which often is initiated from some type of acute pain). These are only a few of the countless situations in which a baseline measure is not practical.
The Brain Gauge does not need baseline measures, which makes it unique amongst sports concussion systems. In peer-reviewed population studies, the Brain Gauge has demonstrated much better sensitivity to the concussion-related symptoms than ImPACT (Immediate Post-Concussion Assessment and Cognitive Testing, a commonly used online tool) and BESS (Balance Error Scoring System, a stability assessment). For more details on that large-scale comparison, you can read about in our published report here (Brain Gauge review) or in a shorter summary here (handout – how BG measures compare). To summarize, the study collected data from 200+ concussed athletes and showed that while Brain Gauge scores were very compatible with clinician return-to-play decisions that averaged 14 days post-concussion (in other words, the average recovery period for a concussed individual from concussion to when they were allowed to return-to-play by the physician was 14 days), the average post-concussion return to baseline score for ImPACT was 7 days (i.e., individuals were determined to be ready to return-to-play on day 7 post-concussion even though they were not actually cleared for another week). The BESS results showed a 15% improvement over baseline by day 3 post-concussion. Given the results of the study, the case study presented below should not come as much of a surprise.
One Car Accident, Two Head Injuries
As we mentioned above, one reason that the Brain Gauge was designed to not depend on baseline measures was because we thought that it would be rare that someone would have a baseline score before something like a car accident and be able to have a pre-injury baseline to compare to. It is rare, but it did happen! Two student-athletes who had recently been baselined for ImPACT and BESS for potential concussion were in a car accident. Both suffered a head injury, and since they were part of a sports program, their head injury was assessed. So how did each student-athlete perform on their concussion tests?
Every head injury is different, even when the injury is from the same situation – and this turned out to be a good example of that. Data is displayed below (both subjects were in the same car). Both people sustained a head injury, but as shown below, the details of their injuries were quite different. Not only were each of them tested with a Brain Gauge post-injury, but they were also evaluated using 2 other concussion tests: BESS (Balance Error Scoring System), and ImPACT (Immediate Post-Concussion Assessment and Cognitive Testing). The Brain Gauge scores from subject #1 demonstrates a significant deficit, and this was consistent with the patient report of moderate neck pain, mild headache, pressure in their head, and difficulty remembering. Patient also had a temporary loss of consciousness after the accident, which is usually indicative of severity of a head injury. How did the patient do on the commonly used concussion tools? On BESS, the patient registered zero errors (i.e., no problems detected). On ImPACT, the patient demonstrated that they were in better shape than they were before the accident (i.e., their scores were better than their pre-injury baseline scores). They even showed an improvement in their reaction time composite relative to their baseline. If you want to read more about errors in reaction time testing with online cognitive tests, you can read about it here.
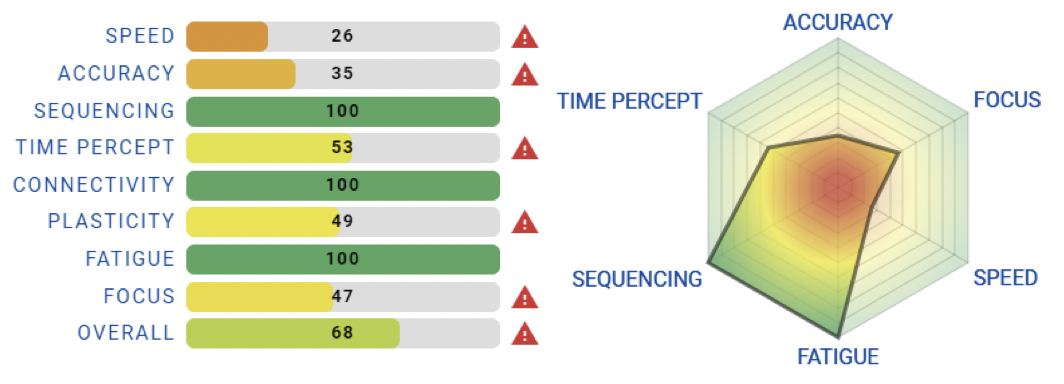
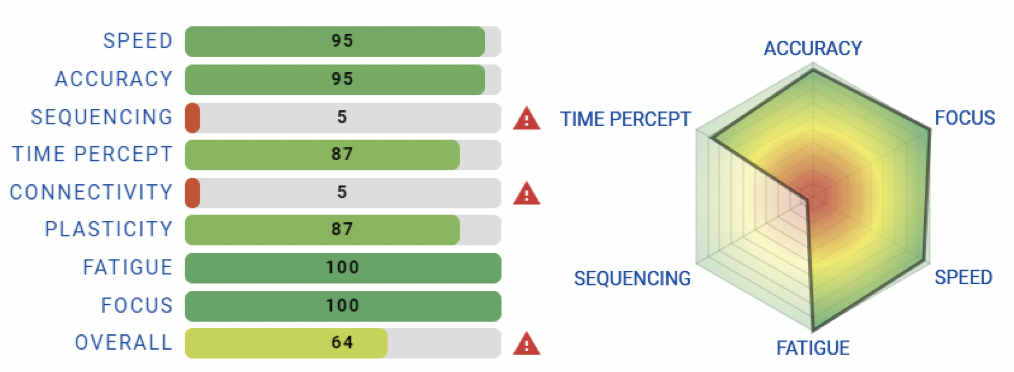
The second patient, although they had no loss of consciousness from the accident, reported severe neck pain, moderate headache, sensitivity to light, having trouble falling asleep, and being more emotional (e.g. higher anxiety) than before the trauma. The Brain Gauge scores reflected some very significant deficits in a couple of scores and the overall composite score was flagged as below normative range. It is interesting to note that patient #2 had symptoms that were slightly different from patient #1 and this was reflected in the Brain Gauge scores. The BESS score for this patient demonstrated a 280% improvement over baseline (yes, they did almost 3 times better than they did before the concussion). They also demonstrated improvements above baseline on ImPACT and the reaction time component of ImPACT.
The one interesting similarity to note between the two injuries is that both of them showed improvement in their ImPACT and BESS scores relative to baseline, and those are the tests that are generally used by health care professionals in the sports world to evaluate when head injury has healed. Both people were clearly not recovered at the time of testing, but the commonly used assessments – ImPACT and BESS – lacked any sensitivity towards showing any brain related injury. In a later post, we’ll discuss why these measures continue to be the mainstay for many sports concussion programs. But until then, we’ll leave it up to you to determine what works best for assessing brain health and how best to gauge what brain health assessment works best for which situation.
